By Jerry Ong
The scale of the COVID-19 pandemic has caught many countries by surprise and the rapid spread has placed a high demand for intensive units and isolated facilities. Flexibility and capacity are key factors in healthcare design.
Read: Looking Ahead: Healthcare Facility Planning for Health Crises
NATIONAL CENTRE FOR INFECTIOUS DISEASES
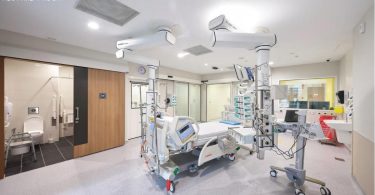
In Singapore, the National Centre for Infectious Diseases (NCID) is at the frontline of the battle against the COVID-19 pandemic. Learning from past outbreaks such as SARS or MERS, the hospital has the ability to swiftly provide the demand for specialised healthcare facilities.
Prior to the opening at the end of 2019, hospital operators had already ramped up operations, run through the standard operating procedures (SOPs) and even treated cases of monkeypox. When the COVID-19 outbreak started, NCID was ready to admit patients in need of intensive care.
Read: NCID and Ng Teng Fong CHI wins three international awards for outstanding healthcare design
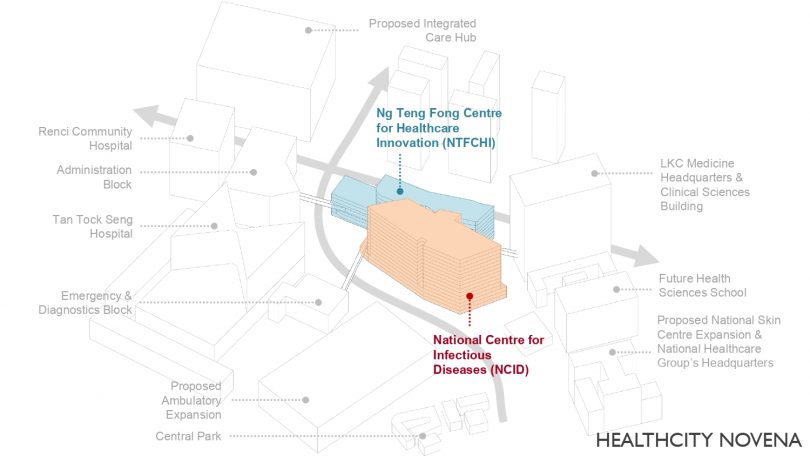
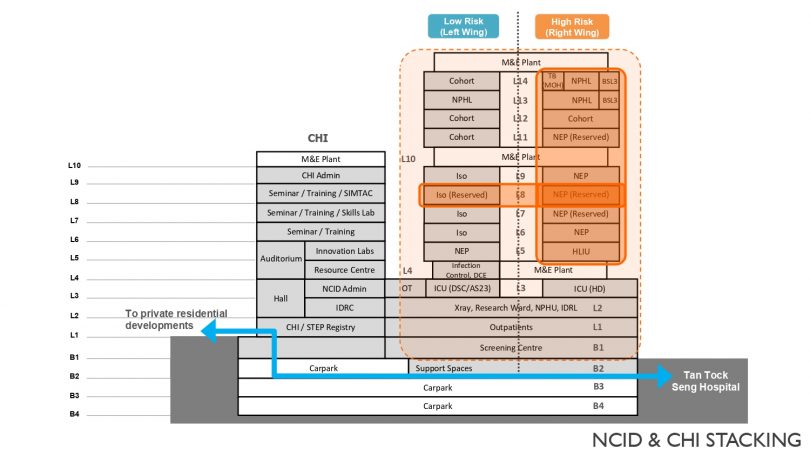
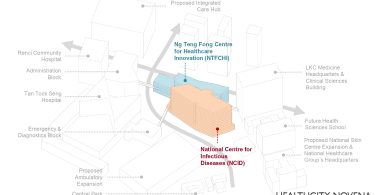
The NCID is located near Tan Tock Seng Hospital, integrated with the future HealthCity Novena Masterplan, where healthcare facilities will be sitting side-by-side with education and training centres such as the Ng Teng Fong Centre for Healthcare Innovation (CHI). In the event of non-pandemic, NCID can be an extension of Tan Tock Seng Hospital and admit any cases of infectious diseases.
Both NCID and CHI function effectively not just as independent entities but also integrated smoothly with its environment, with close connection to the surrounding buildings of Tan Tock Seng Hospital and the Lee Kong Chian School of Medicine via link bridges and underpasses.
REMARKABLE TRANSFORMATION ABILITY
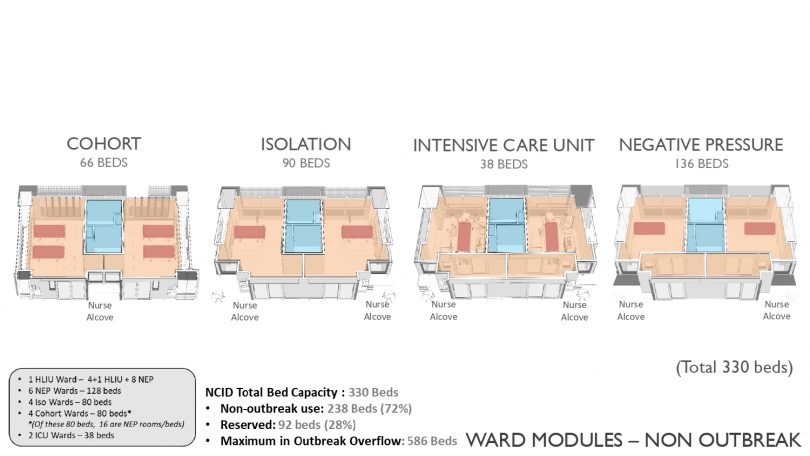
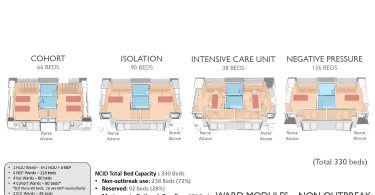
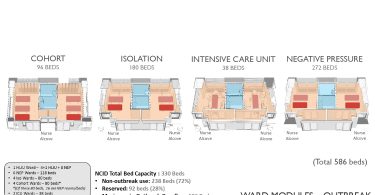
Despite NCID being a specialised high-end type of facility, it still achieves the highest Green Mark Platinum rating with 33.7 per cent of energy savings. The inpatient facilities consist of 17 wards with 330 beds including:
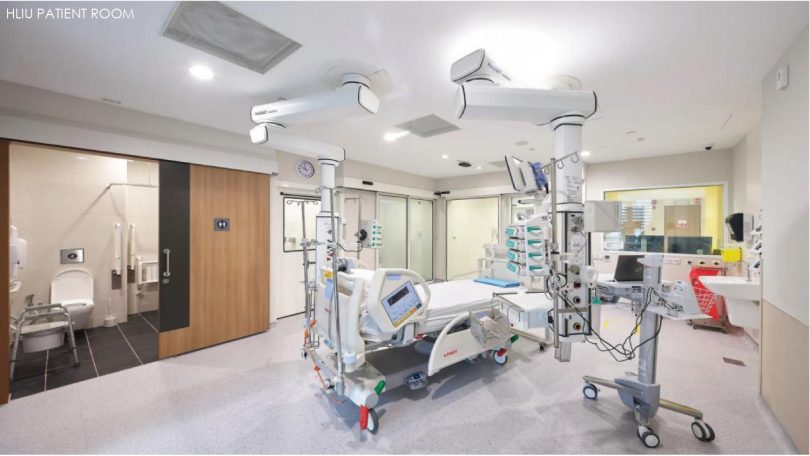
- 1 High level isolation ward with 4 high level isolation units (HLIUs) and 8 negative pressure beds
- 5 Negative pressure wards with 100 beds
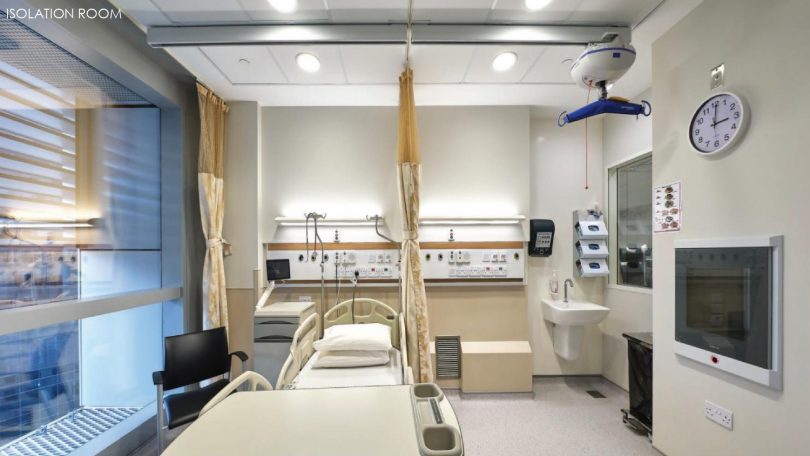
- 5 Isolation wards with 100 beds
- 4 Cohort wards with 80 beds, including 16 negative pressure beds
- 2 ICU wards with 38 beds
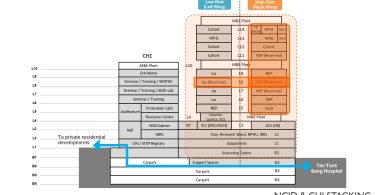
The NCID is also lauded for its transformation ability in resolving complex service design challenges in dealing with the major health crisis. Every ward in each wing can be converted into an isolated area, and so can the whole floor or the entire wing. This lends the hospital the flexibility to deal with different outbreak scenarios. And even if the whole hospital is being locked down, the thoroughfares linking the facilities and Tan Tock Seng Hospital, as well as the neighbouring residential areas, can still be maintained 24/7. The residents can make their way through the buildings via underground routes without compromising their safety.
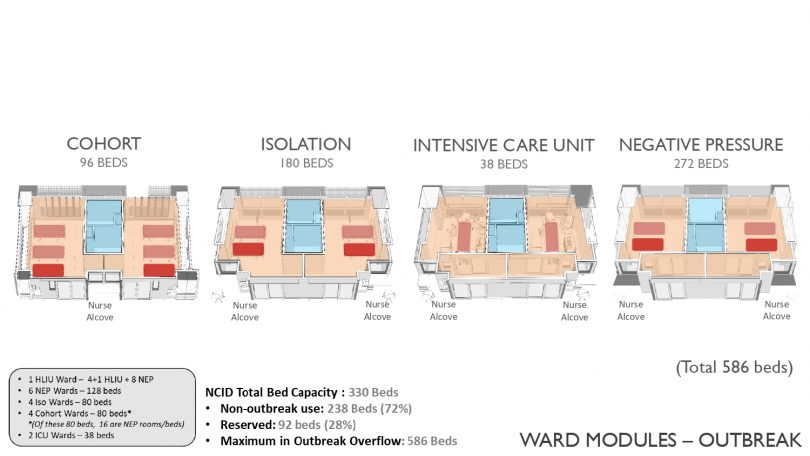
All the wards are designed flexibly in modules for conversion, be it the cohort, the isolation, the intensive care or the negative pressure unit. Beds can be added when the need arises so the capacity can be increased from 330 to 586 beds. Originally designed to face the potential Ebola outbreak, certain wards can also be converted into HLIU facilities complete with support rooms, a laboratory and a decontamination zone.
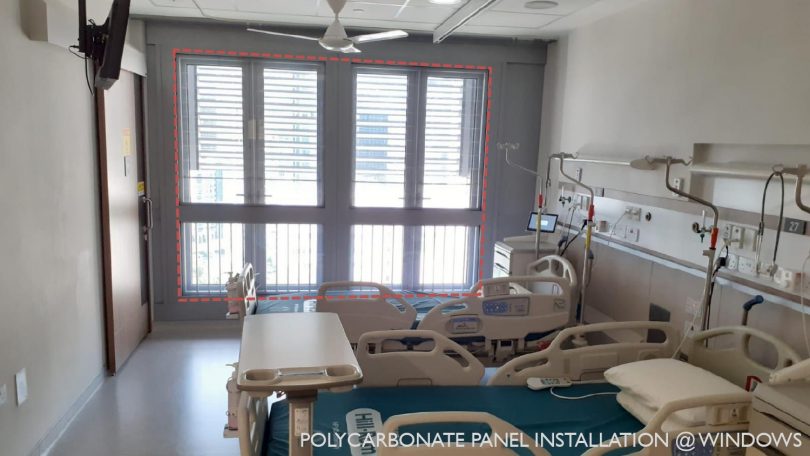
The patient rooms were previously designed as naturally ventilated rooms with louvres. To convert them into isolation units, the louvre and the façade were sealed using a polycarbonate panel before the room was negatively pressurised.
The conversion was accomplished rapidly. A day after the first COVID-19 patient was reported in Singapore on 23 January 2020, the protocols for NCID ward conversion were activated. After the WHO declared COVID-19 a global emergency on 30 January 2020, the conversion work started on 7 February 2020 and was completed on 15 February 2020.
Read: Jerry Ong and Saurabh Bhagra on crisis-ready healthcare design
OCCUPANTS’ SAFETY
Each ward and floor are able to operate independently thanks to the dedicated lifts for patients and materials. Access for visitors is through the central area, where they remained in a lounge before being led into the facility. At the back, there are dedicated circulation routes for staff and logistics. There is a clear segregation of people and materials flow and a safe and thorough waste management system.
The overall M&E system also operates independently. The airflow design is a single-pass air-conditioning system without recirculation, with separate air-handling units supplying fresh air to different zones. Exhaust air passes through HEPA filters before it is dispersed into the atmosphere.
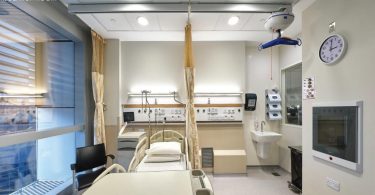
The ward is designed to treat cases of different severity. It is set up, for example, to allow for staff to conduct minor procedures and also to monitor patients without direct contact so as to minimise the risk of transmission.
CONCLUSION
The COVID-19 pandemic has reinforced the need for our healthcare facilities to be more flexible, resilient, and capable of rapidly increasing capacity to deal with an influx of patients in need of various treatments. Hospital design, therefore, must be robust and integrated with the surroundings.
There is undoubtedly a capital cost to provide this additional capability, but in such times when the lives of many depend on proper facilities and services, this kind of capital cost will pay off. Front-liners will be protected, cases can be handled properly, and spread of infectious diseases can be minimised. – Presented to Construction+ by Jerry Ong; reported by Anisa Pinatih
About the presenter:

Jerry Ong is a Senior Vice President (Architecture) with CPG Consultants Healthcare Division and a key member of the team for National Centre for Infectious Diseases and Centre for Healthcare Innovation in Singapore. He also leads the design team to develop masterplan and design proposals for international projects such as the 250 bed Sime Darby Medical Centre ParkCity in Kuala Lumpur, Malaysia and Indus Medical Campus in Karachi, Pakistan. Jerry was also the key project architect for the multiple award winning Khoo Teck Puat Hospital @ Yishun. For his efforts in the development of sustainable hospital designs, Jerry was awarded the Green Building Individual Award (Commendation) by the Building and Construction Authority (BCA) in May 2013. He was also identified as one of Singapore’s 15 great engineers and architects aged 40 and under by Singapore Business Review in 2015. More recently, Jerry was identified as one of ‘20 under 45’ Architects under the Architecture & Urban Design Excellence (AUDE) programme of the Urban Redevelopment Authority of Singapore.