Jerry Ong is a Senior Vice President (Architecture) with CPG Consultants Healthcare Division and a key member of the team for the National Centre for Infectious Diseases and Centre for Healthcare Innovation in Singapore. He also leads the design team to develop masterplan and design proposals for international projects such as the 250 bed Sime Darby Medical Centre ParkCity in Kuala Lumpur, Malaysia and Indus Medical Campus in Karachi, Pakistan. Jerry was also the key project architect for the multiple award winning Khoo Teck Puat Hospital @ Yishun. For his efforts in the development of sustainable hospital designs, Jerry was awarded the Green Building Individual Award (Commendation) by the Building and Construction Authority (BCA) in May 2013. He was also identified as one of Singapore’s 15 great engineers and architects aged 40 and under by Singapore Business Review in 2015. More recently, Jerry was identified as one of ‘20 under 45’ Architects under the Architecture & Urban Design Excellence (AUDE) programme of the Urban Redevelopment Authority of Singapore.
Saurabh Bhagra is a Senior Principal Architect with CPG Consultants Healthcare Division. He was the lead architect for the National Centre for Infectious Diseases and Centre for Healthcare Innovation from the earliest design stages in 2012 to the completion of the facility. Saurabh is currently working on the development of the Office Headquarters (MOH-HQ) for Ministry of Health, Singapore. The MOH-HQ, envisioned as the future workplace for Healthcare Agencies in Singapore is designed with a strong focus on wellness and human centric approach in a highly flexible, resilient and responsive work environment. Saurabh is currently leading a multi-disciplinary global project team and stakeholder management on this project.
The National Centre for Infectious Diseases (NCID) and Ng Teng Fong Centre for Healthcare Innovation (CHI) won international healthcare design awards for their high levels of sustainability and urban integration, as well as for their transformative ability in resolving complex service design challenges in dealing with the COVID-19 pandemic. Construction+ interviewed Jerry Ong and Saurabh Bhagra to talk about the award-winning facilities’ rapid conversion to deal with the surge in demand for treatments during the outbreak in Singapore.

Has there been feedback from the healthcare professionals or patients on the sustainable and integrated design of NCID?
JO: After the official opening, which was immediately followed by the fight against COVID-19, we haven’t managed to do post-occupancy survey with the occupants and operators. We would like to engage with them after COVID-19 subsides to assess the areas that can be improved. For the time being, we’re still in an on-going fight, but we have received some feedback.
The key takeaway is that there may be unforeseen variable between the design and the real use of a healthcare facility. For example, the temperature was designed to be optimal. We set it to be between 23 and 24 degree Celsius (°C) for the daily operation of the facility. However, when the staff were in the facility, they had to use protective personal equipment (PPE) that is made of unbreathable material so they felt hot even when the temperature was set in 23 to 24°C. To allow the staff to feel more comfortable, the temperature had to be lowered to 18 to 19°C. But then again, for the patients, this was too cold. And I think Saurabh can recall his own experience, which was treated as a suspected case in the facility.
SB: Yes, it was very cold! In March 2020, when I came back from London, I was a suspect case of COVID-19 and got referred to NCID. This was my first time visiting NCID as a patient and not as the architect for the project. On my arrival at the screening centre, I could see patient queues starting at the drop-off. From outside I saw many patients wearing white sheets and wondered if it was some kind of PPE. The moment I cleared the triage I could really feel the cold. Soon it all became obvious; the white sheets were actually blankets that were keeping the patients warm. The temperature was set low and this was understandable because, like Jerry said, the patients were in a transitionary process to get their check-ups, but the staff in screening centre were working long shifts and their comfort was critical to 24/7 functioning of the facility. There were so many patients coming in, so you can imagine how difficult it must be for the staff to work continuously in a heightened state wearing all those layers of PPE.
To return to your question about what makes NCID so special, I think besides the immense value NCID adds to our health system, it truly demonstrates that effective infectious diseases planning and management is possible in dense urban neighbourhoods. Even today, NCID maintains a 24/7 campus connectivity in Healthcity Novena while it leads the COVID-19 response in Singapore.
Pandemic Scenario Planning has to be embedded in design and operations. NCID was designed with carefully thought-out scenarios that balanced health safety and business continuity. We can strengthen our healthcare eco-system by ensuring that our facilities are designed to meet these changing operational needs. That level of planning in design and operation need to come through. By the end of it, it gives you sense of assurance and safety that no matter how difficult the circumstances are, there is a safe place where you can be treated. I came back from a highly exposed area, London, to Singapore on that day. God forbid but if I was exposed, NCID would be the only place I would want to be in. That really brings up confidence and trust in the system.
Further to add on Jerry’s on feedback from NCID, I agree that is a continuous learning journey. NCID was designed pre-COVID-19. The design was influenced by experiences from SARS, MERS, H1N1, Ebola and other global outbreaks. With each outbreak we learn something new. So will be the case for COVID-19. This outbreak has had much more impact on the world than any other recent outbreak. Expectations will change and there will always be a need for improvement. With this COVID-19 outbreak, the clinicians, the doctors and operators will learn and improve their process. Their feedback will be very important to innovate future healthcare facilities. As the pandemic response is still ongoing, we are yet to hear the feedback from the clinicians and operators at NCID. We will engage them further for post occupancy surveys to make improvements and adopt them in our future design.
Read: National Centre for Infectious Diseases (NCID): Healthcare facility planned for crises

During the outbreak, did NCID only treat COVID-19 patients or any other infectious diseases?
JO: What I understood is that most of the patients were already been transferred out of the facilities to prepare for the influx of COVID-19 patients. This building was designed from the experience of SARS, which is what we call as a medium-scale outbreak. Even with the expandable capacity, it was still not enough to deal with the number we were looking at. During the pandemic, NCID was dedicated for those who suffered from severe cases and needed more dedicated care.
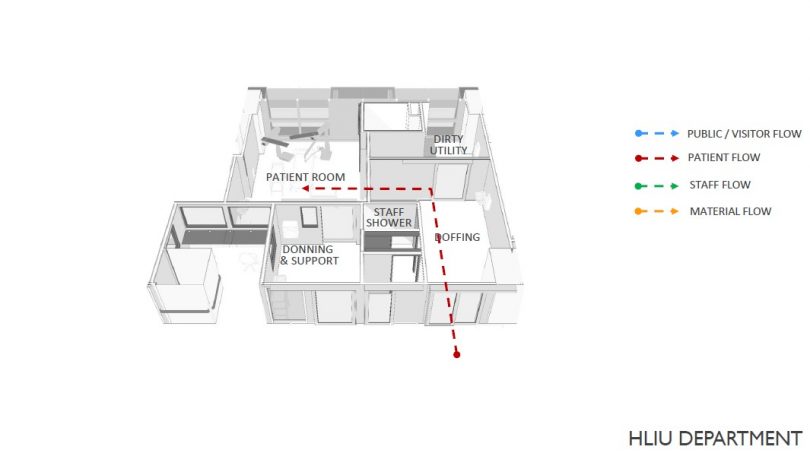
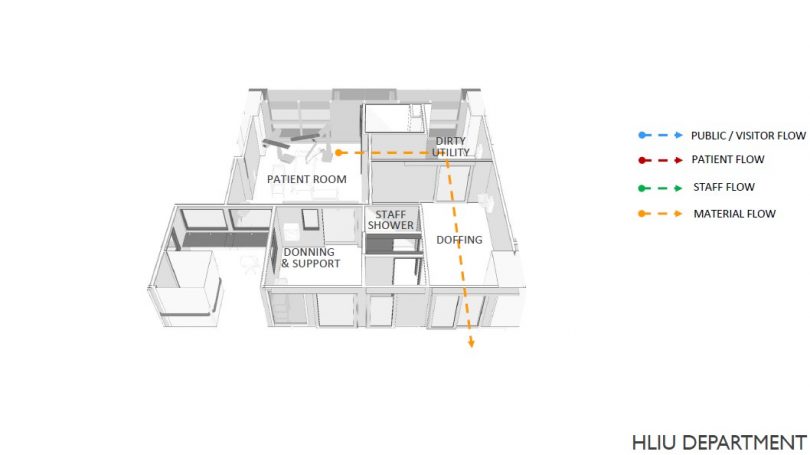
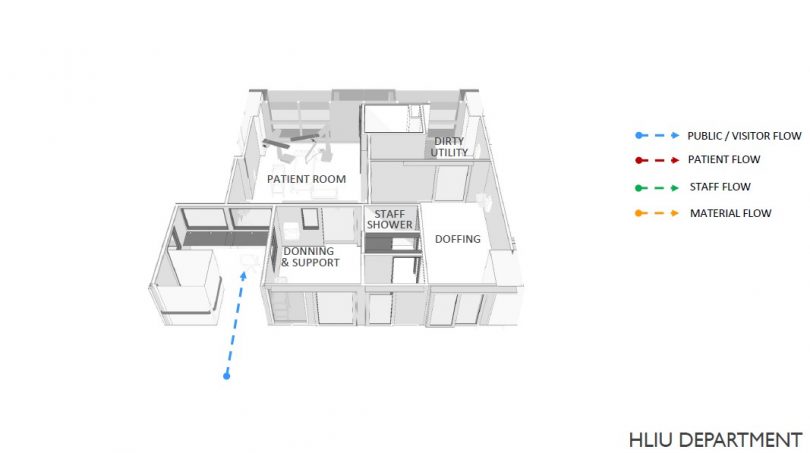
SB: The facility is designed to handle multiple outbreaks of varying severity, but as the scale and impact of COVID-19 was overbearing, the entire facility was dedicated to treat COVID-19 patients. NCID provisions for different types of patient rooms that range isolation and negative pressure rooms to highly specialised units such as the high-level intensive unit (HLIU) that can be used to isolate and treat Ebola cases.
Please elaborate on the technicality of the conversion of the units.
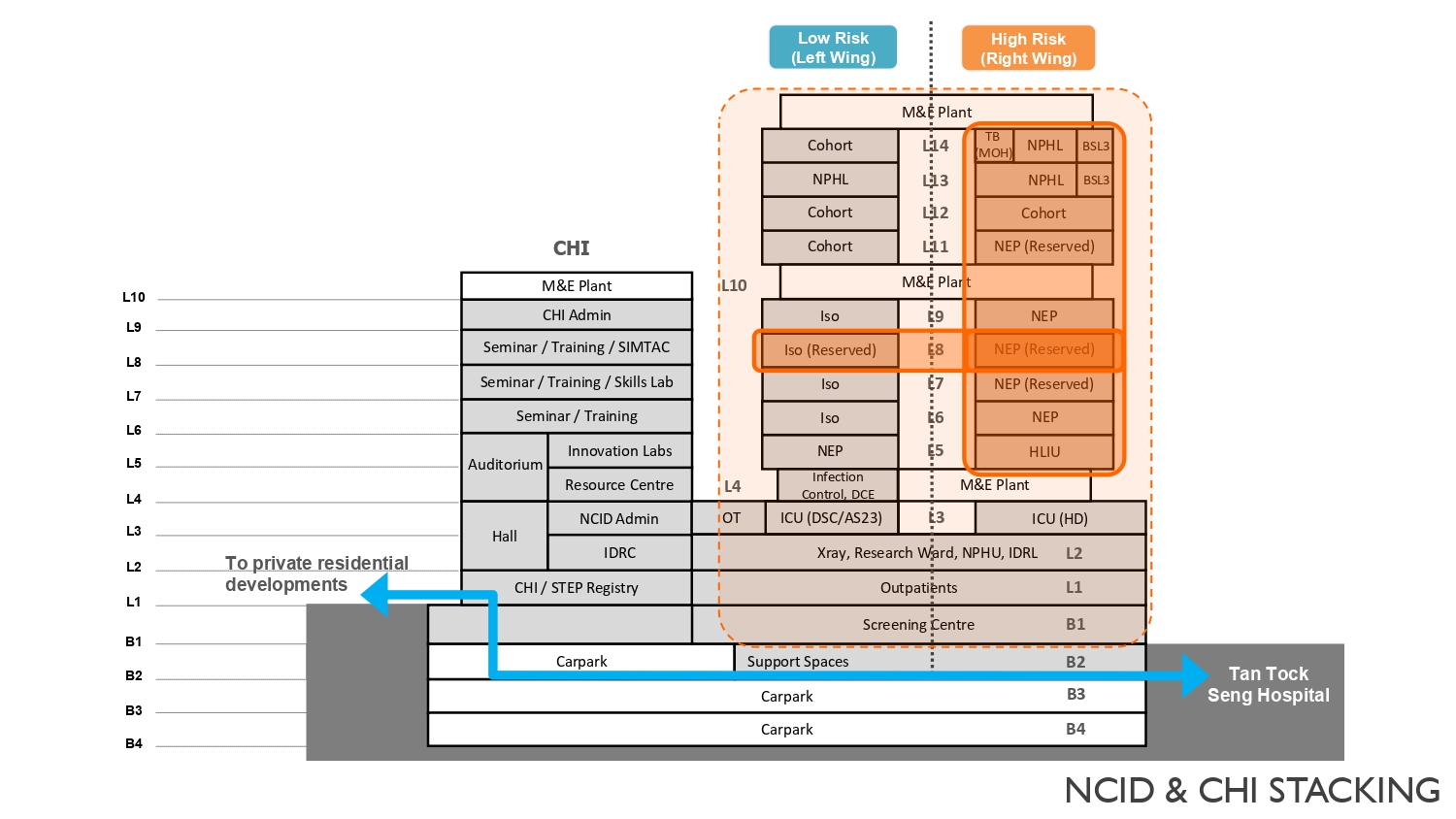
SB: The wards are designed with a modular concept to enable future conversion of one type of ward into another with minimal renovations and without impact to the major structures. The left wing is designated for the low-risk cases and the right wing for the high-risk cases. Some of these wards are naturally ventilated but during times of outbreak, these are converted into negative pressure rooms. For example, to convert the six-bedded cohort ward we used a demountable wall at a pre-determined location to create two isolation rooms. Before commissioning these isolation rooms, our team conducted a series of air regime and smoke pressure tests to ensure a safe environment for staff and patients. During the current COVID crisis, 32 isolation rooms were converted across four wards in a span of only nine days.
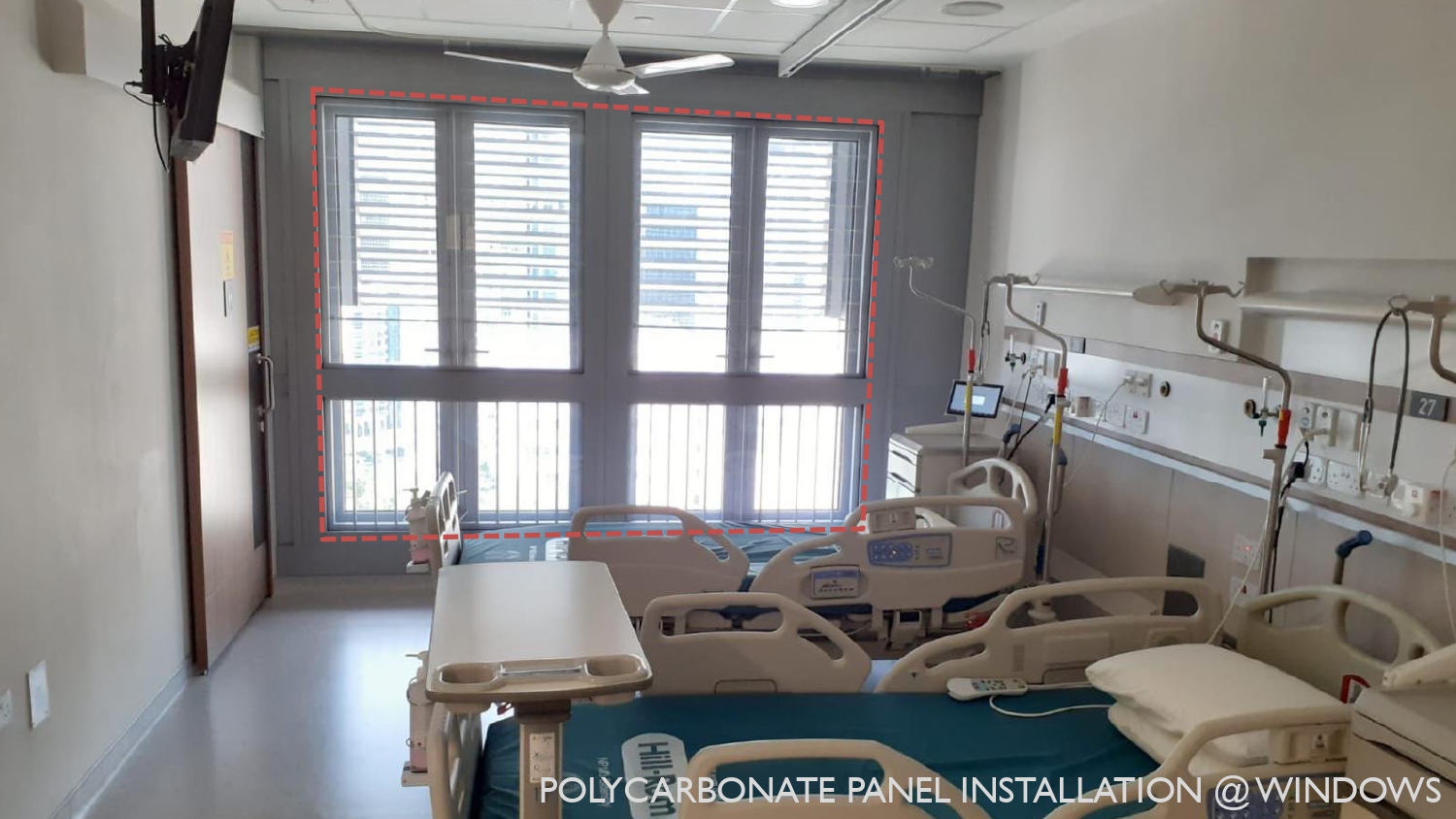
In times of outbreaks the patient areas are considered dirty and the staff needs to be protected by careful design of the airflow within the facility. This means that there has to be a directional air flow from clean to dirty areas.
The conversion of naturally ventilated to negative pressure rooms means that we need to seal up all the glazing. NCID has been designed with a high-performance airtight façade. Air leakages can compromise negative pressure environments and lead to mould growth through water vapour build-up in the facility.
JO: Just to be clear, this will not be successful if we have not designed for this conversion from day one. It is just that we never expected it to be implemented. The pandemic is unforeseeable. It is not to say that this kind of conversion can be easily done in any facilities that have not been designed for it.